Scripps Health | Hospitals and Clinics in San Diego
Here for You
With online scheduling for access to primary care physicians, specialists and state-of-the-art facilities at more than 30 locations throughout San Diego County, we’re here for you.
Public Notice: Scripps Mercy Hospital Chula Vista and Scripps Mercy Hospital San Diego OB services consolidation. Learn more here.

Virtual Care
If seasonal outdoor activities lead to minor injury, our telemedicine options quickly get your questions answered. Consider a Video Visit to talk with a doctor or nurse practitioner today.
News and Articles
View our latest news, videos and health tips

Scripps Encinitas Named Among Top 100 Hospitals in the US
Scripps Memorial Hospital Encinitas was the only hospital in Southern California to make PINC AI's prestigious list this year.

New Treatment Option for Low Back Pain Makes Headlines
A new minimally invasive procedure offers an alternative treatment to low back pain with BVN nerve ablation. Scripps expert explains the procedure.

Scripps Health Leaders Included in Becker’s List of Chief Medical Officers to Know in 2024
Anil Keswani, MD, and Ghazala Sharieff, MD, MBA, recognized for their innovative initiatives around patient care.
Play It Safe: Sexually Transmitted Diseases Are on the Rise
Sexually transmitted infections continue to rise. Learn the symptoms, risk factors and treatments for gonorrhea, chlamydia and syphilis.

Dispelling 9 Myths About Organ Donation
Get the facts about common organ donation myths, from religious concerns to being too old to be an organ donor and more.
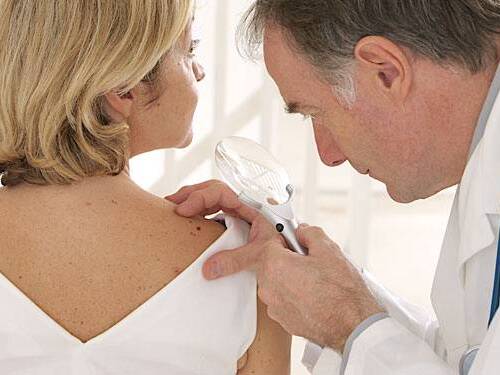
How to Prevent Skin Cancer
Skin cancer is largely preventable simply by reducing exposure to the sun’s UV rays, A Scripps dermatologist offers sun safety tips.





