Stroke Quality Data
Stroke quality measures and outcomes
Stroke quality measures and outcomes
Stroke is a medical emergency that requires rapid treatment — the more quickly you receive care, the better your chances of survival and long-term recovery. You can also reduce your risk of serious side effects, including permanent disabilities, by seeking care from hospitals that have proven their ability to manage even the most complex stroke cases.
Scripps Memorial Hospital La Jolla was one of the first US hospitals to receive Comprehensive Stroke Center certification by The Joint Commission. Scripps Mercy San Diego Hospital has received a certification by The Joint Commission as a Thrombectomy Capable Stroke Center. These elite designations mean we offer a high standard of stroke care not available at many hospitals, including minimally invasive treatments that can reopen blocked arteries, seal a ruptured blood vessel or remove a blood clot from the brain.
Additionally, Scripps’ other hospitals with emergency rooms are all certified as Primary Stroke Centers by The Joint Commission. This means if you or a loved one ever need stroke care, you can rest assured that Scripps has the advanced protocols and procedures in place to treat you quickly and effectively.
Below is some important data illustrating Scripps’ experience and performance in treating stroke patients during the 2022 fiscal year.
Volume and types of stroke patients
Scripps cares for a large number of stroke patients and has the experience necessary to diagnose and treat all varieties of stroke, no matter how complex.
Number of stroke patients treated at Scripps (FY2023)
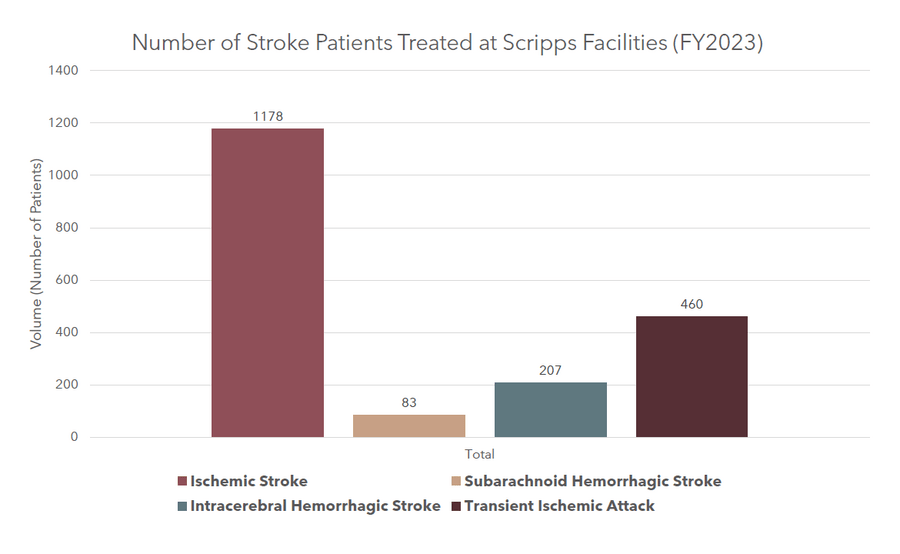
Number of stroke patients treated at Scripps (FY2023)
Inpatient performance measures
Scripps utilizes evidence-based guidelines endorsed by The American Heart Association and American Stroke Association, to ensure all patients suffering from stroke receive appropriate care. At Scripps, we monitor our compliance with our stroke core measures as endorsed by The Joint Commission. The chart below highlights our consistent performance in exceeding standards.
Scripps stroke core measure composite compliance (FY2023)
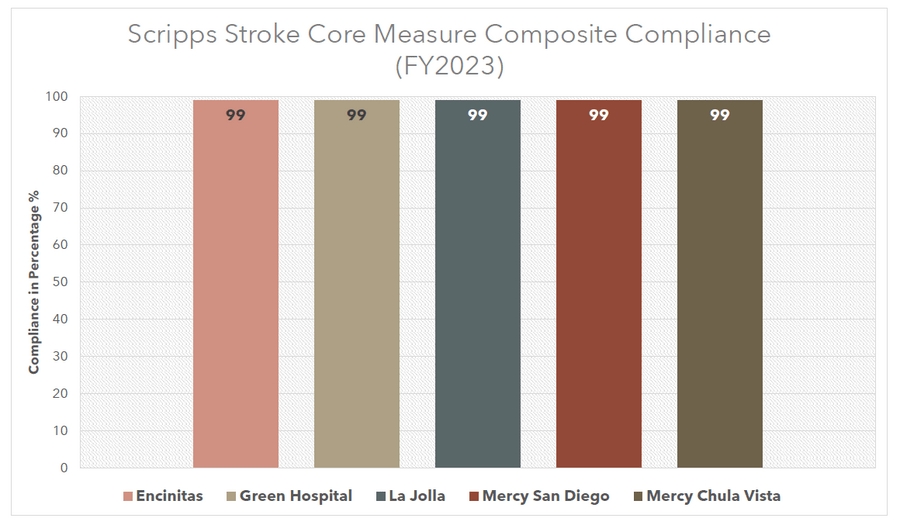
Scripps stroke core measure composite compliance (FY2023)
Amount of time it takes to administer IV Alteplase (tPA)
Time is brain! Clinical practice guidelines recommend hospitals administer a type of clot-busting medicine called tPA to eligible ischemic stroke patients within 60 minutes of arrival.
Scripps has been recognized with the Target: stroke elite plus honor roll and the Target: stroke elite honor roll award by the American Stroke Association for using thrombolytic therapy within 60 minutes in 75% or more of applicable acute ischemic stroke patients.
Effectiveness of endovascular procedures
Ischemic strokes are caused by a blockage in one of the arteries that supply blood to the brain. Patients with evidence of blockage in one of the major blood vessels in their brain, who present within the first six hours from the onset of their stroke, can be treated with a catheter-based approach. This endovascular treatment immediately restores blood flow, captures the blood clot and removes it from the blood vessel.
Successful reperfusion after endovascular treatment after ischemic stroke (FY2023)
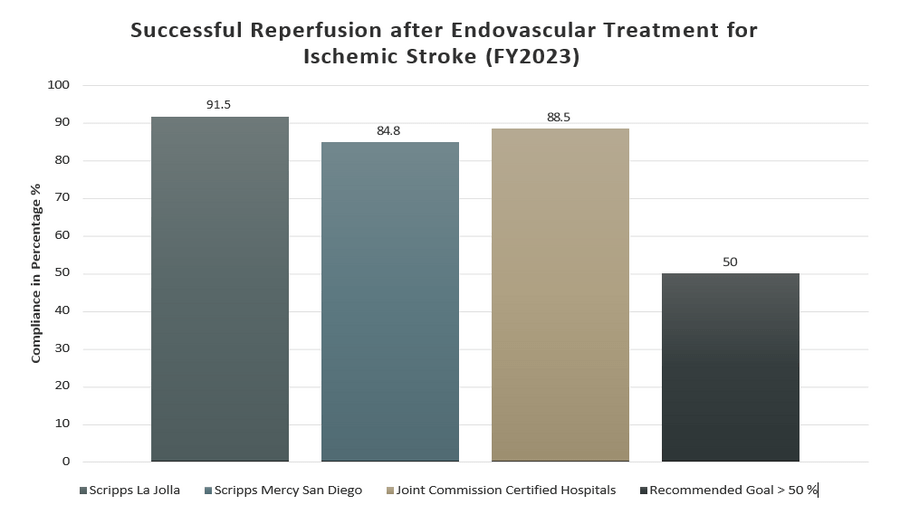
*Recommended goal from the Endovascular Stroke Standards Committee of the Society of Vascular and Interventional Neurology (2015)
Successful reperfusion after endovascular treatment after ischemic stroke (FY2023)
Many hospitals use a scale called thrombolysis in cerebral infarction (TICI) to evaluate the success of endovascular treatments. The more open a blood vessel is following treatment, the more easily blood can flow through it.
In 2015, the Endovascular Stroke Standards Committee of the Society of Vascular and Interventional Neurology established the following national benchmark for hospitals: At least 50% of ischemic stroke patients who undergo endovascular treatment must achieve a TICI grade of “2b” or higher. This means the vessel completely fills with blood, even though the rate of blood flow may be slower than normal.
Scripps La Jolla and Scripps Mercy Hospital San Diego exceeded this goal, achieving TICI scores of 2b or higher among 90% of patients treated with endovascular procedures.