
An innovative pacemaker gets Whitney DeSpain back on track. Read Whitney's story.
Fill out the form to request a referral to a Scripps heart care expert.
Leading-Edge Heart Care, Centered Around You
At Scripps, nationally recognized heart care means more than expertise — it means care that’s designed specifically for you. Our team of specialists uses the most advanced technology and diagnostics to create personalized, effective treatment plans. From prevention and early detection to innovative, minimally invasive procedures and rehabilitation, we're partners in your care every step of the way.
You can trust your heart to Scripps
We believe exceptional heart care starts with truly knowing our patients. Our compassionate, patient-centered approach focuses on treating the whole person — not just the illness. We work closely with you to understand your unique needs, so you can feel confident and informed throughout your treatment process.
Consistently ranked by U.S. News & World Report as one of America’s Best Hospitals for cardiology and heart surgery, we offer innovative heart care for you and your family throughout San Diego County.

Paul Teirstein, MD, Interventional Cardiology, Scripps Clinic
Diagnosing and treating common heart care conditions
Discover why Scripps is a top choice for heart care
Scripps has been trusted by the San Diego community for more than 100 years.
Scripps is consistently ranked by U.S. News & World Report as one of America’s Best Hospitals for cardiology and heart surgery. Our physicians are also recognized as leaders in advanced, minimally invasive techniques and breakthrough research, making Scripps a top choice for heart care.
The Prebys Cardiovascular Institute at Scripps is one of the largest, most advanced centers on the West Coast for cardiovascular medicine, research and training. Through a longtime partnership with Kaiser Permanente, Scripps also is the exclusive provider of cardiac surgery and interventional cardiology surgery to Kaiser Permanente members in the San Diego region.
With nearly 200 affiliated cardiovascular doctors and a network of clinics and hospitals throughout San Diego County, Scripps offers patients a comprehensive range of heart screening tests, diagnostic exams and treatment options.
Additionally, each of our hospital emergency departments has been recognized by the American Heart Association as a certified STEMI receiving center. Our protocols exceed national standards in rapid response time and adhere to national best practices for heart attack care to improve chances of survival and recovery.
Scripps continues to transform medicine in unprecedented ways through technologically sophisticated procedures — many of which are available nowhere else. Frequently, these procedures are performed by physicians who have earned international acclaim for cardiac care.
The Scripps cardiovascular team includes a wide range of experts to address your medical needs, from the common to the complex. Whether you need a routine check-up, advanced diagnostic testing or heart surgery, we can help you get back on the road to health — and stay there.
We’re leading the way in cardiac advancements, interventional cardiology, women’s heart disease, wireless heart care and more.
Some of Scripps cardiology “firsts” include:
- One of the first coronary stents — was co-invented by Scripps Cardiologist Richard Schatz, MD
- First in San Diego to use pulsed field ablation to treat atrial fibrillation
- First in San Diego to utilize catheter ablation to cure arrhythmias
- First in San Diego to use approved cryoablation (cold) technology to cure atrial fibrillation
- First in the United States to implant a dual-chamber defibrillator
- First noninvasive peripheral vascular lab in the US
At Scripps, we treat the person, not the illness. You’re at the center of a team of heart specialists whose common goal is to maintain or improve your heart health.
Our patient-centered approach to care includes experts in preventing, diagnosing, managing and treating heart disease. We keep you and your loved ones informed and involved every step of the way, from helping you understand your diagnosis to making educated decisions about your treatment.
We also know that you have concerns that go far beyond your medical treatment. We’re committed to doing all we can to help you, with comprehensive support services, including rehabilitation services, integrative medicine, palliative care and referrals to numerous community resources.
Exploring heart care locations across San Diego County
Prebys Cardiovascular Institute

Prebys Cardiovascular Institute
9888 Genesee Ave.
La Jolla, CA 92037
Scripps Mercy Hospital San Diego

Scripps Mercy Hospital San Diego
4077 Fifth Avenue
San Diego, CA 92103
Scripps Clinic John R. Anderson V Medical Pavilion

Scripps Clinic John R. Anderson V Medical Pavilion
9898 Genesee Ave.
La Jolla, CA 92037
Scripps Memorial Hospital Encinitas

Scripps Memorial Hospital Encinitas
354 Santa Fe Drive
Encinitas, CA 92024
Scripps Memorial Hospital La Jolla

Scripps Memorial Hospital La Jolla
9888 Genesee Ave.
La Jolla, CA 92037
Scripps Clinic Carmel Valley

Scripps Clinic Carmel Valley
3811 Valley Centre Dr.
San Diego, CA 92130
Scripps Clinic Rancho Bernardo

Scripps Clinic Rancho Bernardo
15004 Innovation Dr.
San Diego, CA 92128
Scripps Green Hospital

Scripps Green Hospital
10666 N. Torrey Pines Rd.
La Jolla, CA 92037

Eric R. received life-saving treatment following sudden heart failure.
Transforming medicine, saving lives
Scripps cardiologists have helped revolutionize medicine — from co-inventing one of the first coronary stents to leading groundbreaking research to providing cardiac procedures that are often unavailable anywhere else.
Learn more about how our cardiologists have impacted the field of cardiology.
One of the most advanced heart care centers on the West Coast, our state-of-the-art heart hospital combines leading-edge technology with patient-centered features to create an atmosphere of well-being and healing.
Our physicians have played a major role in advancing medicine including developing the stent, gene therapy, transcatheter valves, dual chamber defibrillators and other revolutionary treatments.
Expert care for women, by women: Scripps Women’s Heart Center physicians empower women to protect their hearts through education, lifestyle, and expert medical care.
Contact us
Take a quick assessment
Are you at risk for heart disease? Take our quick assessment and see if you may be at risk.
Related News
Prebys Cardiovascular Institute Marks 10 Years of Heart Care

Prebys Cardiovascular Institute Marks 10 Years of Heart Care
From minimally invasive valve therapies to leading cardiac research, see how Scripps Prebys advanced heart care over the past decade.
Scripps MD First in County to Fix Leaky Aortic Valve With New Device
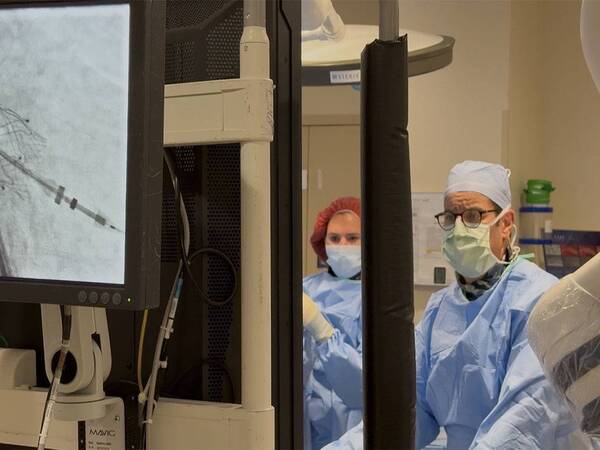
Scripps MD First in County to Fix Leaky Aortic Valve With New Device
Patients have a new option following the recent approval of the first transcatheter aortic valve replacement implant to treat severe aortic regurgitation.
Oral Health and Heart Disease: Why Gum Disease Matters

Oral Health and Heart Disease: Why Gum Disease Matters
Gum disease may raise heart disease risk through inflammation and bacteria. Learn the warning signs. Protect your oral and heart health.
Scripps Cardiologist Explains New Cholesterol Guidelines

Scripps Cardiologist Explains New Cholesterol Guidelines
During an interview with Fox 5 TV, Scripps Clinic cardiologist Elizabeth Epstein, MD, discussed what these changes mean, especially for younger people.
What to Do If You Have High Blood Pressure

What to Do If You Have High Blood Pressure
What causes high blood pressure (hypertension)? Learn the symptoms, how it is diagnosed and why treatment is important to prevent heart attack and stroke.
Is Red Meat Bad for You?

Is Red Meat Bad for You?
Eating too much red meat may raise heart disease and cancer risk. Learn how often you should eat it and healthier options.
